What is Mohs Surgery?
Mohs surgery is a highly skilled and precise surgical technique, developed by, and named for Dr. Frederick E. Mohs. Mohs surgery is used for the management of numerous types of skin cancer including basal cell carcinoma and squamous cell carcinoma and is the treatment of choice for certain basal cell and squamous cell cancers of the skin.
Not all skin cancers will qualify for treatment with Mohs surgery. Mohs surgery is most commonly used to treat skin cancers on the head and neck. It is the treatment of choice for cancers that have recurred or re-grown in a prior scar, have poorly defined edges, are particularly large, are aggressive appearing under the microscope, or are in a cosmetically sensitive area.
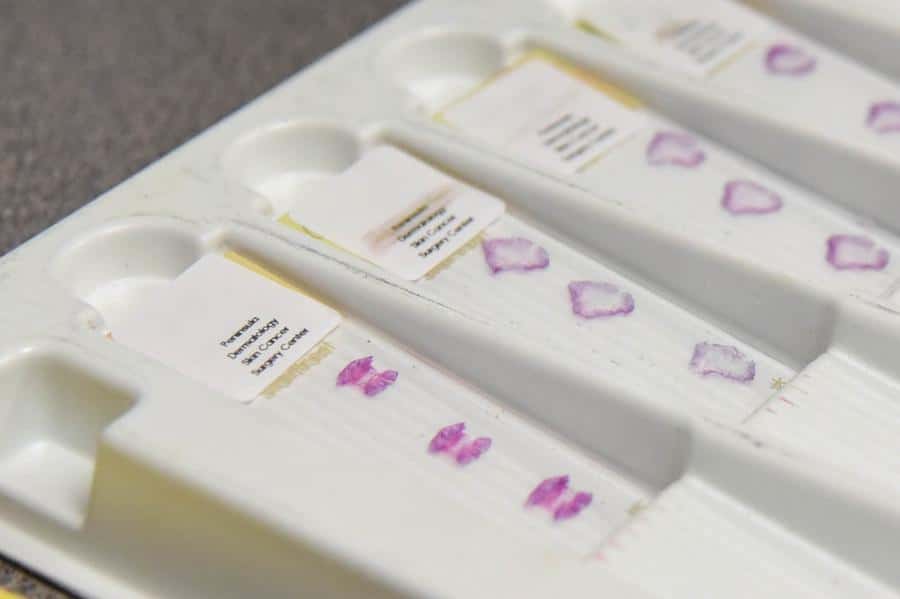
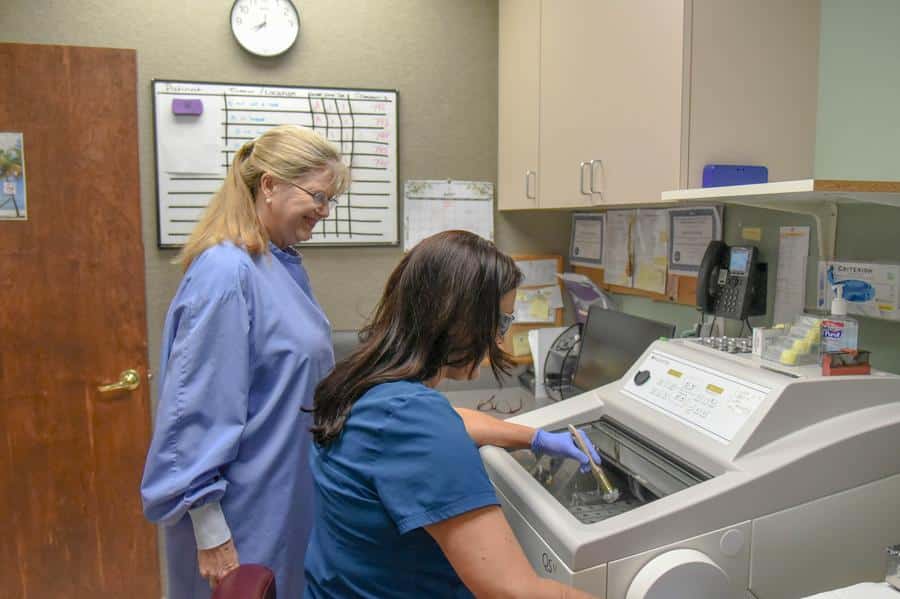
Skin cancers are removed in small sections, one layer at a time. The removed tissue is examined under the microscope, in our state-of-the-art high-complexity tissue processing laboratories, to precisely map out any remaining tumor to be removed.
Mohs Surgery yields the highest cure rates possible for numerous forms of skin cancer. Patients treated with Mohs surgery to treat basal cell carcinoma and squamous cell carcinoma will have cure rates of up to 99%, while at the same time offering maximal preservation of normal skin, resulting in the best functional and cosmetic outcome. Surgery to remove skin cancer will result in a scar. Mohs surgery will help minimize the amount of scarring by removing the least amount of normal skin necessary to remove the skin cancer while at the same time resulting in the highest cure rate possible.
Reconstruction following the Mohs procedure will often be performed the same day by your Mohs surgeon, though your surgeon may work with other specialized consultants in certain instances.
Mohs surgery is an out-patient procedure performed in our offices by our fellowship trained Mohs surgeons, Dr. Marcuson and Dr. Mazzurco. For more information, please call our office or visit the American College of Mohs Surgery Website. All procedures are performed in our out-patient facilities. All surgeries, including biopsies, are performed by our physicians only.
Watch to learn more about Mohs Micrographic Surgery.
Watch and learn the important role sunscreen plays in helping prevent skin cancer.
Watch and learn the about the importance of catching Melanoma early with screening.
SKIN CANCER

At Peninsula Dermatology Skin Cancer Surgery Center, we offer comprehensive skin cancer care to include diagnosing and treating skin lesions, monitoring patients who have had melanoma, basal or squamous cell carcinoma, utilizing total body photography to monitor patients with abnormal moles and melanoma, as well as education and discussion of techniques for preventing future cancers.
It is well known that sun damage to the skin has a cumulative effect. Over time, the accumulation of sun exposure causes the DNA in skin cells to mutate or change, growing out of control and forming a mass of cancer cells.
Skin cancer is the most common type of cancer. If you have been diagnosed with skin cancer, it is critical to obtain an accurate diagnosis of the type of cancer so that the treatment options will be the most effective.
The American Cancer Society recognizes numerous types of skin cancer including the three most common:
• Basal Cell Carcinoma
• Squamous Cell Skin Cancers
• Melanoma
Your skin cancer will need to be treated. Different treatments are used depending on a number of factors including the type of cancer, the location of the skin cancer, size, histologic features, if the cancer has been previously treated and your personal medical history. Most of these skin cancers can be treated in the office using a local anesthetic.
Your dermatologist will help determine which treatment is the best for you and your skin cancer.
COMMON SKIN CANCERS
Basal Cell Carcinoma
This cancer begins in the basal cells located in the lower epidermis of the skin. Of all of the skin cancers, the basal cell carcinoma (BCC) is the most common.
Squamous Cell Carcinoma
Squamous cell carcinoma (SCC) occurs in the squamous cells located in the epidermis, or the topmost layer of skin and most often in sun exposed areas.
Melanoma
Melanoma is one of the most serious forms of skin cancer. It is more likely to grow, spread and cause significant health consequences if it is not caught and treated early.
REQUEST AN APPOINTMENT WITH OUR SKILLED DOCTORS TODAY
We deeply value the relationships we create with our patients and look forward to caring for you and your family.
Please note that we are accepting new patients, but that new general dermatology appointments are currently scheduling significantly further out.
NEWPORT NEWS
LOCATION

11844 Rock Landing Drive, Suite B
Newport News, VA 23606
Phone: (757) 873-0161
Fax: (757) 873-0205
WILLIAMSBURG
LOCATION

1601 Commonwealth Avenue Williamsburg, VA 23185
Phone: (757) 259-9466
Fax: (757) 259-7907
OFFICE
HOURS

Monday-Thursday:
7:30am-5pm
Friday:
7:30am-4pm